On arrival to the operation room, all eligible participants had an intravenous cannula in situ and monitors according to ASA guidelines. Patients were excluded if they had a history of rheumatoid arthritis, renal impairment, liver disease, had undergone prior back surgery, were on any anticoagulant, or had any other contraindication for spinal anesthesia.Īll patients were informed and consented to receive either iPACK block + ACB (iPACK group n=40) or periarticular LIA block + ACB (LIA group n=40) after spinal anesthesia. The inclusion criteria were having an American Society of Anesthesiologists (ASA) classification of I–III, being ≥18 years old, and having a body mass index (BMI) of ≤50 kg/m 2. E-20-4819, from King Khalid University Hospital, Riyadh, Saudi Arabia), this study was carried out from September 2020 to March 2021. After obtaining Institutional Review Board approval (No. The trial was registered at # NCT04565093. 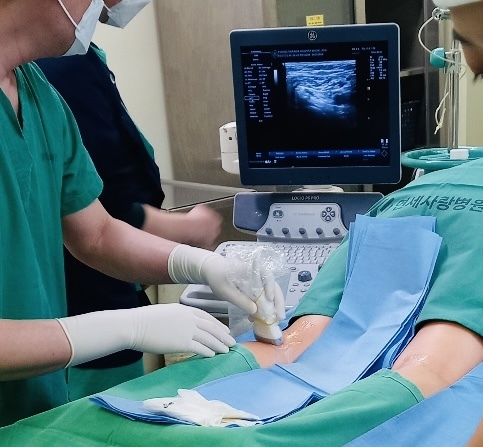
We performed a prospective randomized controlled trial among patients who underwent elective, primary unilateral TKA under spinal anesthesia. We hypothesize that iPACK is an effective technique to provide adequate analgesia after TKA. 16 Therefore, provided the potential advantage of motor-sparing and may be comparable analgesia of iPACK, this study aimed to compare iPACK block with routine periarticular LIA block when combined with adductor canal block (ACB) under spinal anesthesia. Its efficacy depends on the technique and the analgesic drugs regime used, but there is no consensus. 
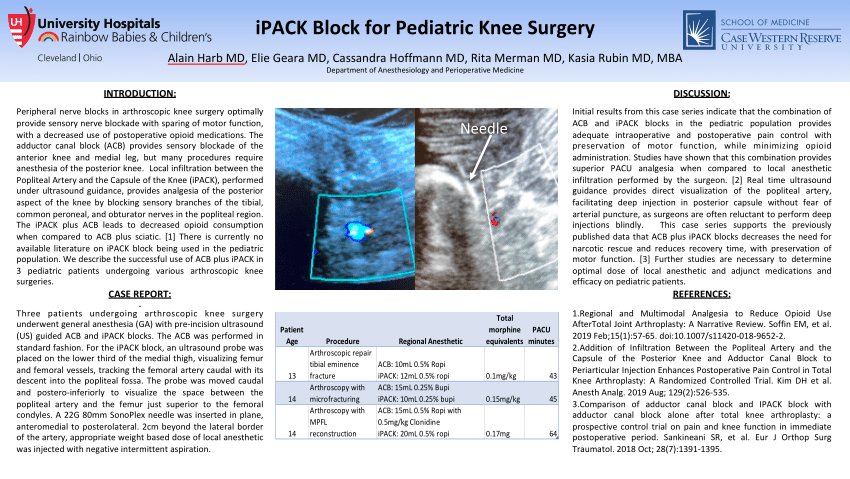
However, LIA block is performed by orthopedic surgeons on landmark technique. In contrast to the local anesthetic infiltration of iPACK, intraoperative periarticular local infiltration analgesia (LIA) is a standard analgesic option for acute pain management after TKA. 15 Unwanted complications during iPACK block include the risk of common peroneal nerve block, intravascular injection, or vascular injury to the nearby popliteal vessels. 13, 14 The advantages of iPACK compare to other modalities for posterior knee pain control are its motor-sparing analgesic effectiveness, reduced postoperative opioid consumption, and improved functional measures. 11, 12 Since the first description of iPACK block by Sinha (unpublished observation)extensive research has been carried out to assess its efficacy. Pain that arises from the posterior knee after TKA may be ameliorated by ultrasound-guided local anesthetic infiltration of the interspace between the popliteal artery and the capsule of the posterior knee (iPACK). 10 The efficacy of blocking these terminal sensory branches at the posterior knee capsule is under investigation. 9 The posterior knee joint is innervated by popliteal plexus, formed by the tibial and posterior branches of the obturator nerves. 3- 5 Alternatively, blocking the saphenous nerve in the adductor canal provides comparable anteromedial pain relief and preserves quadriceps strength comparing to FNB after TKA. Femoral nerve block is an effective technique to control anteromedial pain and reduce postoperative opioid consumption post TKA but results in quadriceps muscle weakness, making physical rehabilitation unsatisfactory. 1, 2 The trend of postoperative analgesia after TKA has been shifted from epidural and femoral nerve blocks (FNB) to motor-sparing sensory nerve blocks. Francis Hospital, Hartford, CT, USA.Optimal pain control and safe postoperative early mobilization are the main objectives of enhanced recovery after total knee arthroplasty (TKA). Sanjay K Sinha, Woodland Anesthesiology Associates in St. This technique was first described by Dr. 
The IPACK block is a muscle strength-sparing technique that consists of an infiltration of local anesthetic into the interspace between the popliteal artery and the posterior capsule of the knee meant to be used as an alternative analgesic supplement to the femoral or adductor canal blocks to cover the posterior knee pain. While the sciatic nerve block results in the best analgesia for the posterior aspect of the knee, motor weakness of the lower extremity preventing early rehabilitation and masking intraoperative common peroneal nerve (CPN) injury do not make it an ideal analgesic modality. What is the rationale for the IPACK block? This month’s addition to the NYSORA web application is the I nfiltration between the P opliteal artery and C apsule of the K nee or the IPACK block. In NYSORA we continue working to create new educational content that combines the latest evidence-based information with requests from NYSORA readers. Table of Contents New Addition: IPACK BLOCK!
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
